An estimated one in ten of the world’s population has a fungal toenail infection, but because feet are easily hidden out of sight, beneath socks and shoes, the problem is often neglected. If unsightly nails are stopping you from enjoying life to the full, the good news is that fungal nail infections can be treated at home, but perseverance is key. If you stop treatment too soon, it will come back.
What causes fungal nail infections?
The commonest cause of fungal nail infection is a skin fungus (dermatophyte) called Trichophyton rubrum. This contagious fungus thrives in warm, humid places, such as bathrooms, changing rooms and communal showers, and loves to infect hot, sweaty feet.
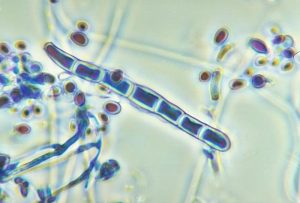
Most fungal nail infections (known medically as tinea unguium, or onychomycosis) are preceded by a fungal skin infection such as athlete’s foot.
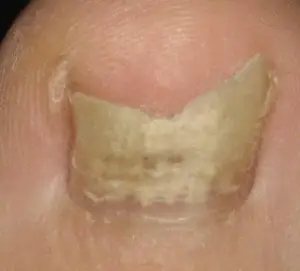
If left untreated, the fungus spreads into one or more nail plates to cause a localised patch of roughened nail that is discoloured and looks yellow, brown or greyish with white patches.
Once a fungal nail infection takes hold, the infected nail may thicken, become brittle and may split to cause pain.
If not addressed, the nail will eventually lift from its underlying bed and, in extreme cases, resemble a claw or horn, and can lead to nail loss. Not an attractive look.
Fungal infections can affect one, several or even all nails of the feet at the same time.
How common is toenail fungal infection?
Toenail fungal infection becomes more common with age, and is also more common among men than women – probably because they are less likely to wear open-toed shoes, or to have regular pedicures or other foot treatments.
One study found the prevalence of fungal foot infection was particularly high among coal miners.
Group
|
% with fungal foot infection |
| All swimmers | 8.5% |
| Male swimmers over 16 yrs | 21.5% |
| Office and shop workers | 14.8% |
| Long-stay hospital patients (male) | 39% |
| Coal miners | 80% |
How to treat toenail fungal infection
As damaged nails cannot be repaired, the aim of medical treatment is not just to eradicate the fungus already present, but to protect the healthy new nail growing through. The new nail plate will look pink and healthy compared to the scarred, discoloured end of the nail which was attacked by the fungal threads.

Treatment must continue until the whole nail has grown through and been trimmed away.
As toenails grow between 1mm and 1.5mm per month, this process can take from 3 to 12 months depending on which nail is affected.
If treatment stops, the fungal infection tends to take hold again and invade any new, healthy nail growth you have achieved, so you have to start over again from the beginning.
Excilor solution review
I highly recommend Excilor Treatment for Fungal Nail Infection which, unlike many other treatments, does not require you to file down the infected nail before application. While filing is designed to help the treatment penetrate the nail plate, it also increases the chance of cross infection to other nails.
 Excilor can treat even deeply embedded fungal growth, and is available as a Pen or a Solution (with brush). It takes just one minute to apply Excilor and one minute to dry.
Excilor can treat even deeply embedded fungal growth, and is available as a Pen or a Solution (with brush). It takes just one minute to apply Excilor and one minute to dry.
The Excilor solution penetrates into the nail and works by increasing the level of acidity within and underneath the keratin nail plate, which inhibits fungal growth and stops it in its tracks.
Excilor is also enriched with oils to moisturise the nail, to help overcome the dryness and brittleness that often accompanies fungal nail infections. Results are visible as soon as the nail starts to grow back.
Keep Excilor by your bed so you remember to apply treatment regularly, every day. If you regularly forget to re-apply the treatment, the fungus will quickly grow into the healthy new nail you have previously achieved.
Preventing a treated fungal nail infection from recurring
The following steps will help stop a fungal toenail infection from recurring after successful treatment.
- Use Excilor 3-in-1 Protector Spray which provides a water-resistant barrier over the skin of your foot (a bit like an invisible sock) to protect against verrucas, warts, bacteria that cause smelly feet, and fungi that cause athlete’s foot and fungal nail infections. The spray claims to protect your feet and toes for a minimum of eight hours.
- Wash feet regularly, especially after exercise, to remove sweaty secretions.
- Dry feet thoroughly after bathing, especially between the toes – use tissue paper or a hairdryer set on gentle heat.
- Change socks or tights daily
- Dust inside shoes and socks with antifungal powder before wearing.
- Wear open toed shoes/sandals when possible – avoid wearing trainers for prolonged periods of time.
- If trainers smell – throw them out and replace them
- Avoid sharing towels or bath mats with someone who has a fungal foot/nail infection.
- Avoid prolonged immersion of nails in water.
- Always apply a base coat before nail polish.
- Sterilise nail clippers and scissors after each use to prevent spreading the infection to other nails.
- Invest in professional pedicures to avoid damaging cuticles and nail folds.
Alternative treatments for toenail fungus
Tea tree oil is a popular topical treatment for toenail fungal infections but is best used in combination with other oils, such as oregano oil, for best effect. Combining Tea Tree oil with Lavender oil is another option, and is more effective against dermatophyte skin fungi than using tea tree oil alone, according to researchers from the University of Derby.
They also found that essential oils of Lemon Grass, Palmarosa, Niaouli and Red Mandarin are highly effective against the common nail fungus, Trichophyton rubrum.
Medical treatment of fungal nail infections
Your doctor can prescribe topical antifungal nail treatments (often a lacquer) that aim to prevent fungal invasion of newly emerging nail. If not used regularly, the new, uninfected nail quickly becomes contaminated and the benefits of previous treatment is lost.
In clinical practice, I have not found prescribed topical toenail fungus treatments are any more effective than Excilor.
If topical treatments fail (usually because of not applying them regularly) your doctor can prescribe an oral anti-fungal treatment. As with topical treatments, pulsed oral therapy is only effective if you remember to take it regularly, as prescribed.
A common oral treatment is itraconazole, taken in pulses (twice daily for seven days, followed by a three-week, drug free period). This pulsed oral treatment is repeated twice for fingernail infections, and three times for toenails. The drug ‘pulse’ saturates the new nail plate, as it is formed, to prevent fungal penetration. Possible side effects of itraconazole include abdominal pain, diarrhoea, nausea, a rash and taste disturbances.
A Cochrane review of 48 studies, involving 10,200 people, concluded that oral terbinafine (once daily) was possibly more effective than itraconazole for achieving clinical cure of fungal toe nail infections and to eradicate the fungus so cultures proved negative. For toenail fungal infection, 12 weeks’ treatment is usually sufficient although a few people may require treatment for up to 6 months. Possible side effects include abdominal pain, diarrhoea, nausea, muscle or joint pains, and headache.
Laser treatment for toenail fungal infection
Laser therapy is available in private clinics to eradicate aggressive fungal nail infections (such as the one shown above) and does so without damaging the nail or surrounding skin.
The laser treatment takes around 20 minutes. In a study involving 250 people, over 70% were fungus-free after a single treatment, but usually two or three sessions are recommended.
Image credits: pixabay; wikimedia; wikimedia; medguy/wikimedia;





