Lower back pain is so common it affects as manly as one in three adults on a regular basis. The good news is that many natural remedies and exercises can improve or even prevent lower back pain. Having worked as a doctor in an orthopaedic clinic for 3 years, I’ve researched the best treatment for lower back pain that can help you avoid strong painkillers or surgery.
Your Backbone
 Your backbone, or spinal column, contains as many as 33 bones and 97 moving joints. The vertebrae interlock in a series of sliding joints that give your backbone flexibility and form four gentle curves that provide extra strength and stability.
Your backbone, or spinal column, contains as many as 33 bones and 97 moving joints. The vertebrae interlock in a series of sliding joints that give your backbone flexibility and form four gentle curves that provide extra strength and stability.
The spinal column is your body’s main support and also surrounds and protects your spinal cord. Due to the complexity of how these bones and joints interlock, and the weight they must support, the only surprise is that lower back pain doesn’t affect everyone.
- 7 cervical (neck) vertebrae support your head
- 12 thoracic (dorsal) vertebrae attach to your rib cage
- 5 large lumbar vertebrae support your upper body
- 5 sacral vertebrae fuse to form the sacrum
- 4 coccygeal vertebrae are fused to form the coccyx (tailbone)
The cervical, thoracic and lumbar vertebrae are separated from each other by pads of cartilage called intervertebral discs.
These have a tough, flexible outer case with a soft, jelly-like centre. Intervertebral discs help to cushion the vertebrae and act as shock absorbers to prevent damage from sudden jolts.
Causes of lower back pain
Low back pain is defined as back pain felt between the bottom of the ribs and the top of the legs. Most cases have no specific cause and are due to excessive strain on muscles, ligaments and small joints.
As well as feeling discomfort from these damaged, strained tissues, the surrounding muscles often go into reflex spasm, too. This means you tend to experience pain and tenderness over a larger area. This spasm may be enough to pull your spine out of shape so that it temporarily curves sideways (scoliosis). This puts excess strain on yet more ligaments and muscles so that a vicious cycle sets up.
As you get older, your intervertebral discs also become increasingly worn and stiff so they are more susceptible to damage. This may weaken the protective outer coat of the disc so the soft, jelly-like core bursts through when under pressure.
The prolapsed centre of the disc often presses on the root of a spinal nerve to cause muscle weakness, pins and needles, spasm and pain in the back. If the prolapsed, or herniated, disc presses on the roots of the sciatic nerve, pain will shoot down your leg to cause excruciating and debilitating sciatica.
Red flag symptoms with lower back pain
Low back pain is rarely dangerous, but signs that there may be nerve damage or pressure and that urgent medical advice is needed include:
- weakness or numbness in one or both legs
- severe pain causing immobility
- pains shooting down the leg
- numbness or pins and needles, especially at the base of the spine or between the legs
- difficulty with, or loss of, bladder control
- difficulty with, or loss of, bowel control.
If any of these symptoms occur, seek immediate medical help. Back pain following more than a minor injury or fall also needs investigation to rule out a fracture or slipped disc. If in doubt, call your doctor’s surgery for advice.
Specific causes of low back pain that need medical attention include sciatica, vertebral facture, abdominal or pelvic conditions that cause pain to refer through to the back (eg urinary tract infections, endometriosis) and, more rarely, conditions such as ankylosing spondylitis or cancer secondaries. If you suspect any of these, also seek medical advice from your doctor.
Immediate treatment of acute lower back pain
Lower back pain that comes on suddenly is referred to as acute lower back pain. If you experience sudden back pain for no obvious reason:
Stop doing whatever caused the pain and ease into a comfortable position. You may find that lying face down on the floor, hands by your side, helps by taking the pressure off your back.
For an acute injury such as a pulled muscle in the lower back, applying an ice pack may help bring relief and limit inflammation.
If the pain is not helped by an ice pack, try applying gentle warmth via a hot water bottle. Warmth is soothing and stimulates blood flow to hasten healing.
For mild to moderate low back pain, stay as active as possible and aim to continue normal daily activities within the limits of your lower back pain. Early mobilisation is essential to stop your back from seizing up. Remaining mobile allows faster recovery and leads to less time off work than resting.
Bed rest is no longer recommended routinely unless your doctor specifically tells you to – studies show that for uncomplicated, acute low back pain, bed rest is ineffective.
Seek medical advice if pain is severe, lasts more than two days, or if you develop numbness, weakness, pins and needles or problems emptying your bowels or bladder as this could mean nerve damage is occurring.
Standard painkillers for lower back pain
Non-specific lower back pain and sciatica is usually treated with simple painkillers, at recommended doses. There are concerns that long-term use of even paracetamol and ibuprofen may increase the risk of heart attack, however, so it’s wise to keep their use to a minimum.
Paracetamol for lower back pain: Until recently, paracetamol was a first line treatment for long-term back pain. Many doctors no longer recommend paracetamol due to recent recognition that its regular use may increase the risk of heart disease (in addition to recognised risks to the liver and kidneys). A US study found that people who frequently consumed paracetamol over 12 years had a 35% increased risk of heart attack or stroke.
A recent Cochrane Systematic Review found that paracetamol was no more effective than placebo for treating acute lower back pain, and it is doubtful that it has any effect on chronic lower back pain, either.
NSAIDS for lower back pain: Non-steroidal anti-inflammatory drugs (eg ibuprofen) help to reduce pain and inflammation, but should not be used long-term. They can cause irritation of the stomach with indigestion or even peptic ulceration.
A recent Cochrane Systematic Review found low quality evidence that NSAIDs are slightly more effective than placebo for treating chronic lower back pain. Six of 13 randomised controlled trials showed that NSAIDs are more effective than placebo in reducing pain intensity, but 7 trials did not.
Paracetamol plus ibuprofen for lower back pain: A recent review of all the evidence found that ibuprofen plus paracetamol was the most effective non-prescription pain killer for most people, with a success rate of around 70%.
Opiate painkillers for lower back pain: Opiate painkillers only work for two-thirds of people as one in three of us inherit genes that affect how they are metabolised, making them ineffective for analgesia. Codeine phosphate is too constipating for more than occasional use. Dihydrocodeine (available over-the-counter in some countries in combination with paracetamol) is limited by its potential for addiction. Talk to the pharmacist before taking these.
Ask your doctor for individual advice about pain relief if your discomfort is severe and over-the-counter painkillers don’t help.
Because of the limitations of painkillers – both those that are prescribed and those that are available from pharmacies – national treatment guidelines for lower back pain and sciatica are moving away from medications.
Non-drug approaches that may be recommended include group exercise programs, physiotherapy, manual manipulation and massage. Psychological therapies such as cognitive behaviour therapy can also help to change the way pain is perceive in the brain, and help you cope with it in a positive way.
Read my full review of oral non-prescription painkillers here.
Read my review of the best topical pain-relieving creams and gels here.
Choose the right mattress for lower back pain
The surface you sleep on is incredibly important and will make the difference between waking up in pain, or waking pain-free. Many people with recurrent back pain sleep on a mattress that is too hard or soft and makes the problem worse. You may have seen advice to sleep on a hard mattress – or even the floor – but this is no longer recommended, and is especially inappropriate for people with arthritis who have other joints that ache, too.
NASA scientists have developed the perfect sleeping surface – a visco-elastic polymer that naturally moulds to your body shape – including the natural curves of your back. This surface was originally developed to help astronauts withstand massive G-forces during space flights. Memory foam mattresses provide firm support as your body sinks comfortably into the material, supporting the natural curves of your back, reducing the load on pressure points and helping your muscles and ligaments recover during sleep.
The reduction of strain on your pressure points also reduces the number of times you turn during sleep from a typical 80 to 100 times a night to less than 20 times. This improves restlessness and pain and reduces the need for sleeping tablets and painkillers.
Mattresses are subject to ageing and the support they provide can deteriorate by as much as 70% from their new state within ten years. If your mattress is overly soft, overly hard, or over 7 years old, it is worth considering a replacement.
If your mattress is in good shape but is too hard, then a memory-foam mattress topper/overlay will solve the problem and can work out cheaper than replacing the full mattress. A memory foam topper can also be rolled up and taken on holiday with you so your back pain doesn’t recur when lying on a strange bed.
Stretch your back to reduce lower back pain
 The vertebrae in your back interlock to form gentle curves, whose sinuous S shape provide additional strength and stability. If these become compressed, the spine is ‘squashed’ or shortened and back pain results.
The vertebrae in your back interlock to form gentle curves, whose sinuous S shape provide additional strength and stability. If these become compressed, the spine is ‘squashed’ or shortened and back pain results.
Stretching exercises will help to free up the back and improve lower back pain.
One of the best spinal exercisers is the Backrack, which was developed by a spinal rehabiliation specialist. It is designed to decompress the natural curves of the spine and to treat both the underlying cause and the symptoms of back pain.
The Backrack is made from ethically sourced wood and is anatomically shaped to help support and realign your back.
Simply lie down on the backrack and the nodules on the spindles will do the rest. They are designed to suspend your spine and to push up under the joints that become compressed. This gentle separates the joints and allows your spine to lengthen and decompress, relieving the pressure that is associated with back pain.
We have kept a Backrack under our bed for over 10 years. My other half regularly lies on it for a few minutes, first thing in the morning, to stretch his back before starting the day. Other back stretching devices are also available.

The Backrack Lumbar Belt for back pain
Designed by the same spinal rehabilitation specialist, the Backrack Lumbar Belt can be worn until your pain and stiffness improves or resolves.
You can wear it while walking, working, sitting at a desk, driving or travelling, to support your back and help relieve the cause and symptoms of lower back pain.
The additional warmth it provides will help you fell more comfortable, and promote blood flow and healing, too.
Other lumbar support belts are also available.
Click here for more information on Backrack products
To get 10% off all Backrack products, use the code EXPSARAH10 when ordering.
Nerve stimulation for lower back pain
Transcutaneous electrical nerve stimulation (T.E.N.S.) is another, drug-free way to relieve lower back pain.
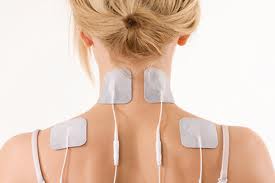 A typical device contains four pads that are stuck to your back, around the area that is causing problems. The device then generates small pulses of electric current that stimulate nerve endings in the skin.
A typical device contains four pads that are stuck to your back, around the area that is causing problems. The device then generates small pulses of electric current that stimulate nerve endings in the skin.
The nerve endings respond by sending continuous messages to the brain, flooding these nerve pathways with the equivalent of low-grade chatter. The brain tends to shut down monitoring of pathways that send constant ‘small talk’ information (in teh same way that you stop smelling your own cologne soon after you’ve put it on) as this ensures it is not distracted from other, more important sensory input.
By down-grading the pain pathways sending messages from the T.E.N.S. machine, the perception of other signals using the same nerve pathways is also reduced. As a result, pain receptors in your back – or wherever you apply the electrodes, is also blocked and your discomfort is temporarily numbed in a similar way to acupuncture.
The Med-Fit 1 Dual Channel Tens Machine, for example, is supplied with 8 electrodes so you can treat two areas simultaneously. Switch between constant, modulation and burst modes, and vary the pulse rate to find which settings work best for your pain.
Acupressure for back pain
Acupressure is an ancient technique that has been practiced in China and Japan for over 3,000 years. Stimulation of certain points on the body reduce pain through physiological effects that, although not fully understood, are undoubtedly effective.
These effects may involve production of the body’s own natural analgesics (eg endorphins), regulate nerve conduction in a similar way to T.E.N.S (above) or – as practitioners believe – balance the flow of life energy along the body’s meridians to prevent blockages associated with muscle spasm and pain.
You can stimulate acupoints by lying on a special mat, or by wearing devices that target a specific acupoint on the leg to help relieve back pain.
Heat packs for lower back pain
Applying heat is one of the best ways to ease lower back pain. The continuous stimulation of heat receptors in the skin has a T.E.N.S. effect to downgrade perception of pain and help numb the area. Warmth also increases blood circulation to boost healing.
Thermacare Heatwraps are worn for 8 hours yet provide up to 16 hours therapeutic relief from lower back pain. This drug free option can be worn discreetly under clothing to provide soothing warmth while you work. The heat penetrates to increase circulation and relax tight muscles and spasm.
Hot packs that can double up as cold packs, are also available.
Hot water bottles for lower back pain
My favourite option for when sitting down, or to use at night, is a hot water bottle. While a traditional small rectangular hot water bottle can fit nicely into the small of the back, I’ve found that a long, thin, hot water bottle offers more flexibility – a long bottle can be wrapped around any part of your torso to help relieve pain. It can also be used as a warm support for your back when lying on your side.
Herbal supplements for back pain
A number of herbal remedies have a medicinal effect to reduce pain and inflammation. They are at least as effective as many prescribed analgesics, but with a lower risk of side effects. That’s not to say they will suit everyone, but they are a valid option now that paracetamol is no longer recommended as a first line treatment. You will soon know how well a particular herbal medicine works for you as an individual.
Rose hip extracts for back pain
Rosehip extracts contain unique galactolipids that reduce pain and inflammation through an aspirin-like effect. They inhibit a group of enzymes (COX-1 and COX-2) that are involved in the generation of pain and inflammation but through a different mechanism that is not associated with aspirin’s well-known intestinal side effects. Rosehip extracts also appear to prevent the migration of inflammatory cells into joints, and to reduce the production of enzymes involved in joint destruction.
A meta-analysis of three studies, involving 287 people, found that taking rosehip extracts for 3 months significantly reduced pain scores, and people taking it for osteoarthritis pain – including backache – were twice as likely to respond to treatment than those taking placebo.
As well as improvements in pain there were significant improvements in morning pain and stiffness, sleep quality, mood, energy and well-being. Taking rosehip extracts reduced the need for rescue medications such as tramadol, codeine and paracetamol.
Turmeric for back pain
Turmeric is an Ayurvedic herbal medicine used to treat joint and lower back pain. The active ingredient is curcumin, a powerful anti-inflammatory antioxidant that suppresses the excessive production of an inflammatory chemical called TNF-alpha. This same substance is the molecule targeted by antibody drugs used to treat osteoarthritis, inflammatory bowel disease, psoriasis and ankylosing spondylitis. These biological drugs must be given by injection – yet turmeric can be taken orally.
Ensure your turmeric supplement is a well-known brand, made to pharmaceutical standards (GMP), to ensure it actually contains the level and purity of curcumin claimed on the label. The curcumin in turmeric that is formulated into liquid micelles is 185 times better absorbed than other forms of turmeric and, as you want optimal absorption to ensure turmeric can act on your lower back pain, this is the form that I recommend.
To read my full review of Turmeric, visit my Nutritional Medicine website.
Devil’s Claw for back pain
Extracts from the root tuber of a South African plant, Devil’s Claw (Harpagophytum procumbens) are a traditional herbal medicine used to relieve back pain. These contain unique substances, such as harpagoside and harpagide, with painkilling actions similar to those of non-steroidal anti-inflammatory drugs but without the same side effects. As well as reducing pain, Devil’s Claw helps to improve mobility.
A Cochrane systematic review of herbal medicines used to treat low back pain concluded that daily doses of Harpagophytum procumbens (devil’s claw), standardized to 50 mg or 100 mg harpagoside, may be better than placebo for short-term improvements in pain and may reduce use of rescue medication. One clinical trial showed that Devil’s claw was as effective as prescribed anti-inflammatory drugs.
Manipulation for lower back pain
Back pain and muscle spasm often relate to misaligned tiny facet joints between the vertebrae. This can be relieved by gentle manipulation from a physiotherapist, chiropractor or osteopath who is experienced and knows what they are doing. If your lower back pain is due to muscle or ligament strains or tears, however, manipulation is less likely to be effective.
Make sure your practitioner is fully qualified and registered with the appropriate chiropractic or osteopathic regulators in your country before entrusting your back to them.
How to prevent lower back pain
Backache is usually due to excessive strain on muscles, ligaments and small joints in the lower back. It is most likely to affect those whose work involves heavy lifting or carrying, and those who spend long periods sitting in one position or bending awkwardly. Many cases of recurrent backache can be prevented by learning the correct way to lift:
- stand close to the load, with your feet either side of it
- squat down by bending at the knees and hips, keeping your back straight and upright
- keep your elbows tucked in and grasp the object with your both hands (not your fingers)
- lean forward slightly and, in one smooth action, straighten your hips and knees while lifting the object and holding it close
- to lower a heavy load, reverse this action, keeping your back straight at all times.
- never combine bending and lifting.
Other back friendly tips include:
- Avoid excess stress which can make you subconsciously tense your back muscles
- Lose any excess weight
- Exercise regularly to strengthen your core abdominal and spinal muscles
- Improve your posture – keep your spine straight when walking and avoid slouching your shoulders
- Sit correctly: keep square on the chair with your bottom well back and your spine upright; use chair arms to take some weight off your shoulders and lower back
- Wear flat or low shoes – high heels change your centre of gravity and affect vertebral alignments
Click here to read about methods of pain relief for tennis elbow.
Image credit: yuganov_konstantin/shutterstock